Upskilling in DED through the BCLA
As an optometrist who specialises in dry eye disease (DED), I am constantly trying to stay on top of the latest research and developments, so it was with great enthusiasm that I embarked on the British Contact Lens Association (BCLA)’s dry eye management and contact lens retention certificate course. Being the first New Zealand optometrist to have obtained this certificate, I feel more confident in my diagnosis and management of DED and more knowledgeable to teach the part V students at the University of Auckland School of Optometry and Vision Science (SOVS).
The learning platform is the BCLA website (www.bcla.org.uk), so you first need to become a BCLA member, which then gives you free access to the course, plus additional resources. You have 12 months to complete all three parts, and I have already applied to ODOB for accreditation for CPD points. Part A comprises five online lectures with a series of multiple-choice questions after each lecture, which must be completed to progress to the next lecture. I have since referred to these lectures many times as they are a premier source of information from world-class lecturers explaining the most up-to-date dry eye wisdom.
Course summary
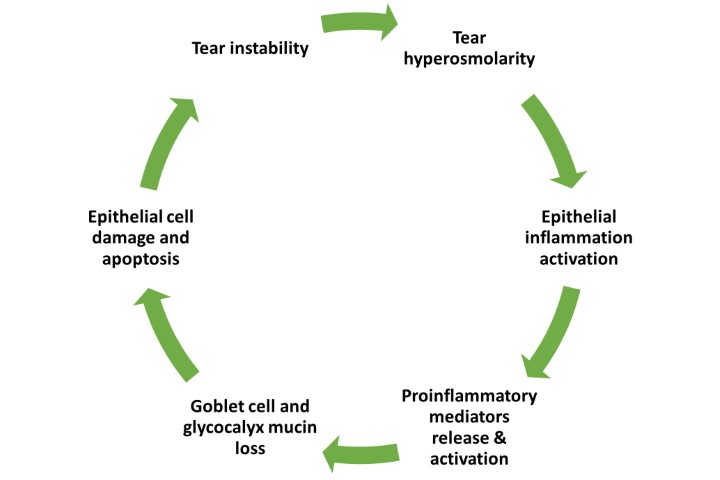
Lecture 1 is given by our very own Professor Jennifer Craig, entitled ‘Classifying dry eye for improved patient care’ and it gives a fantastic synopsis on how to incorporate TFOS DEWS II in clinical practice. It expands on the risk factors to be aware of, reviews the updated definition of DED and thoroughly explains the pathophysiology of the self-perpetuating cycle of the disease.
Lecture 2 is presented by Professor James Wolffsohn from Aston University, UK, entitled ‘Diagnosis of DED’. He reviews the important triaging questions, risk-factor analysis and tests required to diagnose and subclassify DED. He expands on the symptom questionnaires, how to best measure tear stability, tear volume and composition, and assessment of damage to the ocular surface.
Lecture 3 delves into the ‘Management and therapy of DED’ given by Professor Lyndon Jones from the University of Waterloo, Canada, and expands on the stepwise treatments necessary to restore homeostasis to the ocular surface. I found it very useful to learn more about environmental modifications we could recommend, a better explanation about the protective role of essential fatty acids to limit the inflammatory response in the body, and tips to obtain success with warm compresses. Prof Jones emphasised that the key to providing suitable treatment relies on understanding the aetiology while acknowledging that with disease progression it is rare that a single therapy will suffice.
Lecture 4 tackles contact lens comfort and dryness and is delivered by Neil Retallic, formerly an optometry teaching fellow at Manchester University, UK, and soon-to-be BCLA president. He discussed how contact lenses affect the tear film and the ocular surface by presenting the progression of contact lens discomfort. If we can predict contact lens dropout, we have a better chance of retaining contact lens patients.
Lecture 5 is a practical culmination of the series entitled ‘How to operate a successful dry eye clinic’ by Sarah Farrant, a UK optometrist in private practice. She highlighted the prevalence of DED and that there is no value in quickly tacking on advice at the end of an eye exam as you won’t achieve patient compliance. Instead, she said, success requires knowledgeable staff, time devoted to patient examination, management and follow-up visits, as well as demonstration of products, and leaflets or follow-up emails for patient reference.
Part B of the course requires completion of an interactive dry eye workshop or peer review and writing a reflective essay on how you will incorporate your learnings into your practice. And lastly, part C is an oral examination, in my case a Zoom call with two international members of the BCLA who presented various patient cases to discuss.
The gift that keeps giving
I would encourage others to consider taking this course as it is very achievable and allows you to feel confident in providing your patients with the best in dry eye treatment. The benefits don’t stop there, though! For those who wish to demonstrate the highest level of expertise in this area, the module can serve as a springboard to completing a BCLA fellowship in dry eye. Also, as a member of the BCLA, I was able to attend its virtual conference in June which opened my eyes to other practitioners around the world who are treating DED and enabling me to be part of a community that continues to practice and research in this exciting specialty area. Not surprisingly, New Zealand is considered at the forefront of knowledge, and I am very proud to be a part of this cohort.
Dr Marcy Tong is a professional teaching fellow at the School of Optometry and Vision Science (SOVS) and lead optometrist at the dry eye clinic at the University of Auckland.