Providing an optometric dry eye service through a pandemic
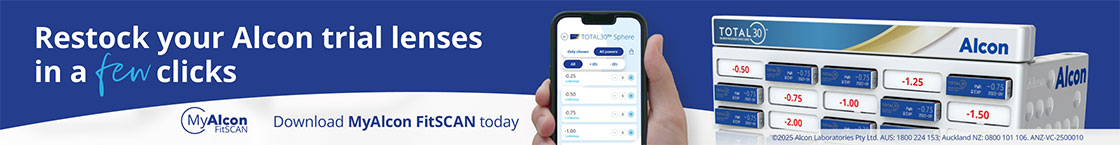
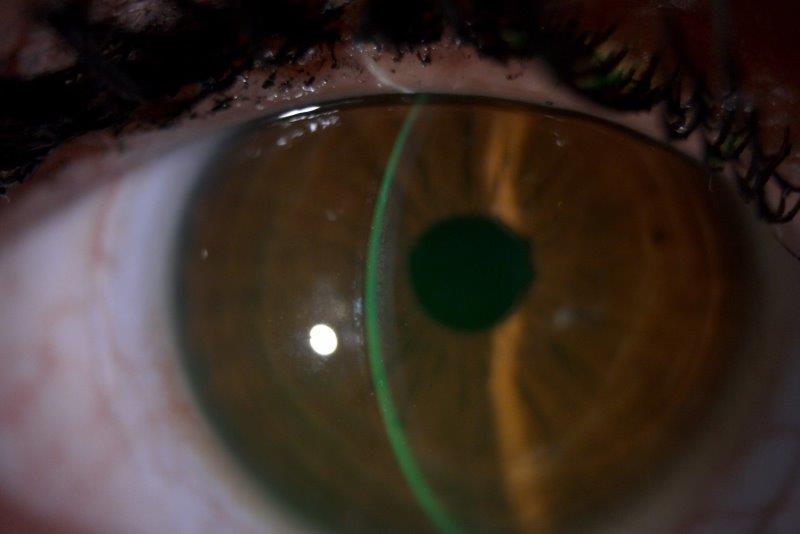
Scotland, like many places, has experienced a cycle of peaks and troughs in Covid-19 case numbers and corresponding restriction levels. I work as part of a wonderful team at Glasgow Caledonian University which has successfully adapted to these changing circumstances. We have an on-site Vision Centre that provides routine eyecare as well as several specialist services, such as the dry eye clinic where we conduct a detailed examination of the lids, tears and ocular surface and tailor patient management appropriately.
Throughout the past year, community eyecare has continued after an initial pause, with triage centres staffed by optometrists to manage all acute problems alongside the hospital eye service. DED can have such a negative impact on quality of life that we didn’t want to leave these patients without care indefinitely. So how have we run our dry eye clinic with these restrictions in place including, at times, during a national lockdown?
Face time
First of all we triaged every patient before inviting them to attend an in-person appointment. Many of the patients on the waiting list when services resumed were routine follow-ups who were managing well and had no new or worsening symptoms. These patients were invited to have a remote consultation with a face-to-face appointment postponed until restrictions eased.
Patients who reported worsening or changing symptoms were given a clinic appointment. New patients, for whom we had no record of diagnosis or ocular surface health, were often invited to attend as well. All of these triage phone calls were made alongside our final year undergraduate students to help them learn about the importance of taking a detailed (and relevant) history and symptoms when managing DED. My colleagues Dr Laura Sweeney and Dr Andrew Logan were instrumental in arranging a rota to ensure weekly clinics went ahead.
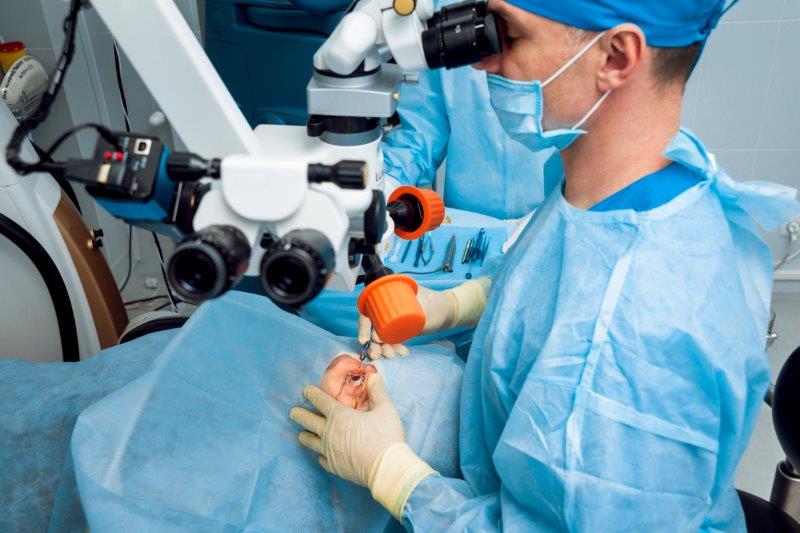
For face-to-face clinics, only one patient attended at any time. This allowed for changes in PPE and cleaning of equipment. This took some getting used to, but we settled into our new routine quickly. Appointment times were also staggered throughout the Vision Centre to avoid patients congregating and they were screened for Covid-19 symptoms by phone the day prior.

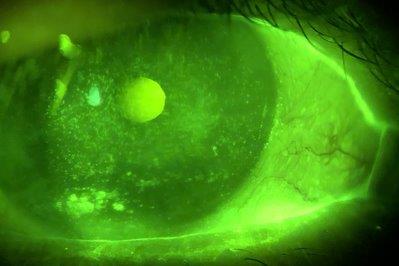
Dr Martin’s colleague Laura Sweeney dons PPE
What struck me most when I saw patients or spoke to them on the phone was how grateful they were for the care; even just a chat to talk through eye drop use was appreciated. This highlighted for our students just how important communication really is, especially in the management of a chronic condition like DED. I should also acknowledge the resilience of our students, in continuing with their education in such exceptional circumstances.
The silver lining
Looking at the positives to have come out of this experience, I see a greater role for optometrists in the community, working collaboratively with our colleagues in the hospital eye service. The success of this model has been demonstrated with the triage centres set up during the pandemic and the use of telemedicine for remote consultations, leading to better networks being established between optometry and ophthalmology.
We’ve also seen more optometrists undertaking further qualifications, particularly for prescribing. During the pandemic this minimised hospital visits and provided appropriate care close to home. There are shared-care schemes starting or expanding throughout Scotland, covering areas such as stable glaucoma care and post-operative cataract care. I see this as becoming the new normal to ensure the best care for our patients in the community.

Dr Eilidh Martin is a lecturer in vision sciences at Glasgow Caledonian University, Scotland. Her research focuses on anterior eye and contact lenses, in particular investigating different aspects of dry eye disease and blepharitis.