OTC focuses on glaucoma
This year’s Ocular Therapeutics Conference has been divided into four ocular therapeutics evenings (OTEs) due to potential pandemic-related interruptions. The theme for the first was glaucoma.
Eye-drop holidays
Auckland Eye’s Dr Shenton Chew’s introductory lecture reinforced the importance of optimising the patient’s quality of life while treating glaucoma. He advised starting a new eye drop in one eye only, so patients can feel the therapeutic effects in comparison to the other eye. This also helps clinicians determine the most suitable medication and dosage. Dr Chew also suggested sending patients on an ‘eye drop holiday’ to help them recover from therapeutic-induced ocular allergies while maintaining glaucoma treatment with oral Diamox (acetazolamide).
He expressed his concerns, however, with prostaglandin-associated periorbitopathy, especially with bimatoprost, as the deepening of the upper lid sulcus can make intraocular pressure (IOP) difficult to measure. His presentation included two important findings from recent studies, the first being that selective laser trabeculoplasty (SLT) is currently the most preferred first-line treatment for primary open-angle glaucoma (POAG) among ophthalmologists, with the ‘Selective laser trabeculoplasty versus eye drops for first-line treatment of ocular hypertension and glaucoma’ (Light) trial concluding that SLT is more cost effective and improves quality of life better than eye drops. The second was that for newly diagnosed POAG patients over 50 years old with an IOP >30mmHg, lens extraction shows higher efficacy and is more cost effective than laser peripheral iridotomy.

Dr Aaron Wong with speaker Dr Graham Reeves
The lasting effects of preservatives
The second talk came courtesy of Eye Institute’s Dr Divya Perumal, who focused on preservatives in glaucoma eye drops and their side effects. Preservatives can damage goblet cells and microvilli of the conjunctiva, which can result in tear film instability and ulceration and can induce apoptosis and failure of the trabecular meshwork (TM). To minimise therapeutic-induced allergies, Dr Perumal advised switching to alternatives that contain fewer irritating preservatives, such as Travopt and Travatan (travoprost), both currently funded in New Zealand. Boric acid, which acts as the preservative in Travopt, is naturally degraded by the cations in the tear film, while Polyquad, which has been used in Travatan since 2011, does not concentrate in contact lenses and is attracted by bacterial cells but repelled by corneal epithelial cells. Extensive studies have shown that preservative-free glaucoma drops improve ocular discomfort and hyperaemia without compromising IOP control. However, in New Zealand there are currently only three preservative-free glaucoma drops available, including Minims pilocarpine nitrate 2%, Lumigan (bimatoprost) – which still causes conjunctival hyperaemia due to prostaglandin analogues – and Ganfort (bimatoprost plus timolol).
Foreign aid
Eye Surgery Associates’ Dr Hussain Patel presented two complex glaucoma cases. The first a 48-year-old Asian woman with retinitis pigmentosa (RP) and severe cystoid macular oedema (CMO). While prednisolone acetate improved the CMO, her IOP was severely raised and continued to rise even after timolol and Diamox use. After attempting different therapeutics but failing to keep both CMO and IOP under control, the patient was able to obtain loteprednol (not available in New Zealand) from Singapore, which kept both CMO and IOP under control. However, sourcing this has become a challenge during the pandemic.
The second case was a glaucoma patient with severe dry eye, meibomian gland dysfunction and blepharitis. The patient was intolerant to all glaucoma eye drops available in New Zealand and surgical intervention was only effective temporarily. The patient was able to tolerate tafluprost (preservative-free travoprost, available in Australia but not New Zealand) but her glaucoma continued to worsen, along with severe dry eye disease, said Dr Patel.
The common theme revealed by these examples is that New Zealand lacks the variety of medications that would be helpful for such special cases.
New therapies roundup
In the fourth presentation, Associate Professor Ilva Rupenthal, director of the Buchanan Ocular Therapeutics Unit which organises the OTE series, introduced new glaucoma therapeutics recently approved by the US Food and Drug Administration (FDA). Rhopressa (netarsudil) is a Rho-associated protein kinase (ROCK) inhibitor, which increases aqueous humour outflow by relaxing the TM and causing a reduction in episcleral venous pressure. It also inhibits norepinephrine transport (NET), which reduces aqueous humour production. A combination drug, Roclatan, containing netarsudil and latanoprost, was also launched, providing additional IOP reduction by increasing uveoscleral outflow. Another recently approved glaucoma eye drop, Vyzulta (latanoprostene bunod), is a nitric oxide (NO)-donating prostaglandin analogue that, similar to other prostaglandins, works by increasing uveoscleral outflow, while NO increases the conventional outflow by relaxing ciliary muscle and TM.
A/Prof Rupenthal also presented a wide range of new drug delivery technologies, including an intracameral implant of bimatoprost (Durysta), a latanoprost microdose delivery device (Optejet) and a punctal plug containing latanoprost (Ocular Therapeutix).
All about the baseline
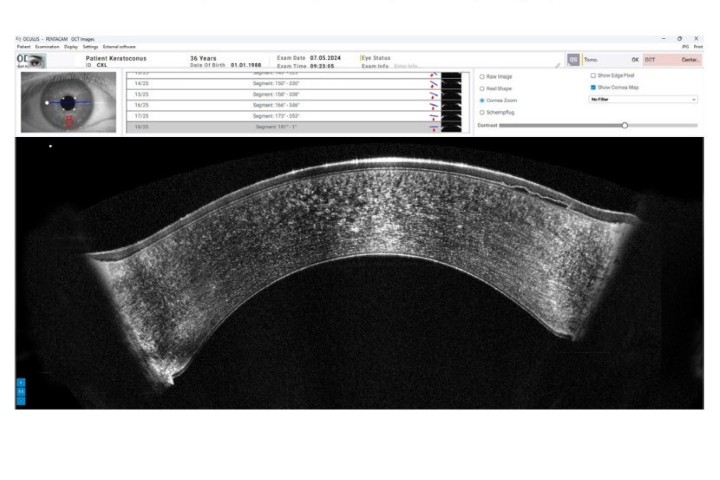
Closing the session, Eye Institute’s Dr Graham Reeves highlighted the importance of interpreting OCT results critically for glaucoma diagnosis and management. Abnormal results can be caused by normal variants and artefacts, such as epiretinal membrane, blinking, hazy cornea, cataract, floaters and small pupils. While progression analysis can be a powerful tool, Dr Reeves reinforced that the results rely on a very good quality baseline scan and repeats should be performed with the same machine. He also presented cases of abnormal OCT results caused by serious underlying pathologies such as pituitary tumour and non-arteritic anterior ischaemic optic neuropathy (NAION).
The next three OTEs will cover anterior segment (12 July), dry eye disease (14 September) and paediatrics (26 October). You can register for any of these here: https://uoaevents.eventsair.com/ocular-therapeutics-evening-series-2021/registration/Site/Register

Charisse Kuo is a therapeutically qualified optometrist in the second year of her PhD at the University of Auckland. Her research involves the development of tissue culture models using human donor retinas and choroids to explore the mechanisms behind sight-threatening diseases.