CASE STUDY: Glaucoma masqueraders
Glaucoma masqueraders (Table 1) are ocular conditions that have clinical features that resemble glaucoma. Like glaucoma, they are conditions that can change the appearance of the optic nerve and may result in optical coherence tomography (OCT) and visual field abnormalities. Some of these conditions may be vision- and/or life-threatening if not diagnosed in a timely fashion. Hence the importance of being aware of glaucoma masqueraders and to have a high suspicion for these conditions when reviewing a patient for glaucoma. It is also important to be aware of key ‘red flags’ that will help distinguish between glaucoma and other causes of optic neuropathy (Table 2).
Case report
A 48-year-old Māori male was referred for a glaucoma assessment due to a suspicious right disc. He reported his right eye had become more blurred over the last year. He was last seen by his optometrist four years prior, with no concerns noted. His medical history consisted of diabetes and hypertension and his medications included Accupril and metformin. He had no family history of eye problems.
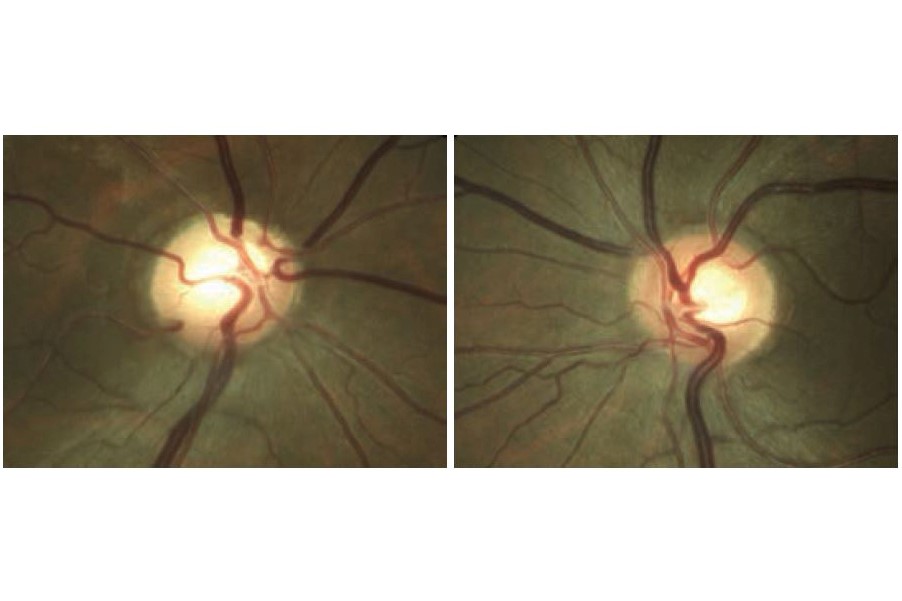
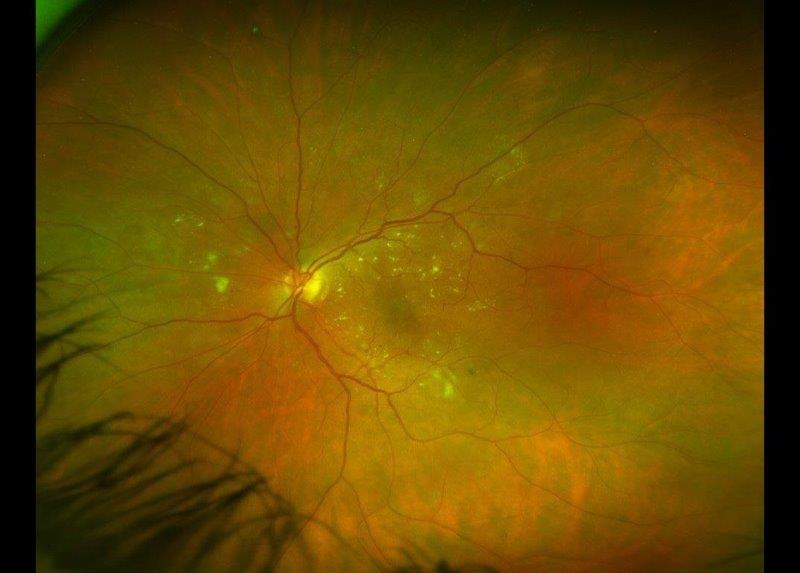
His best-corrected visual acuity (BCVA) in the right eye was 6/12 and in the left eye 6/6. His intraocular pressures (IOPs) were 13mmHg bilaterally and corneal thickness measurements were 543μ right eye and 540μ left eye. He was noted to have a mild right relative afferent pupillary defect (RAPD) and abnormal Ishihara plate testing on the right (9/14 OD, 14/14 OS). His anterior segment examination was normal and drainage angles open. The optic discs are presented in Fig 1 and demonstrate cupping and pallor affecting the superior right disc. His visual fields (VFs) showed a dense inferior altitudinal field defect on the right.
This patient had many concerning features for a non-glaucomatous optic neuropathy, including his age and ethnicity, reduced vision, RAPD, decreased colour vision, disc pallor and altitudinal VF loss. Subsequent neuroimaging demonstrated an internal carotid artery aneurysm compressing the right optic nerve.
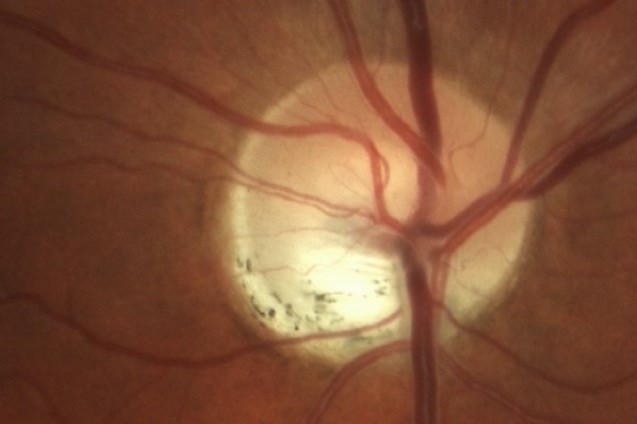
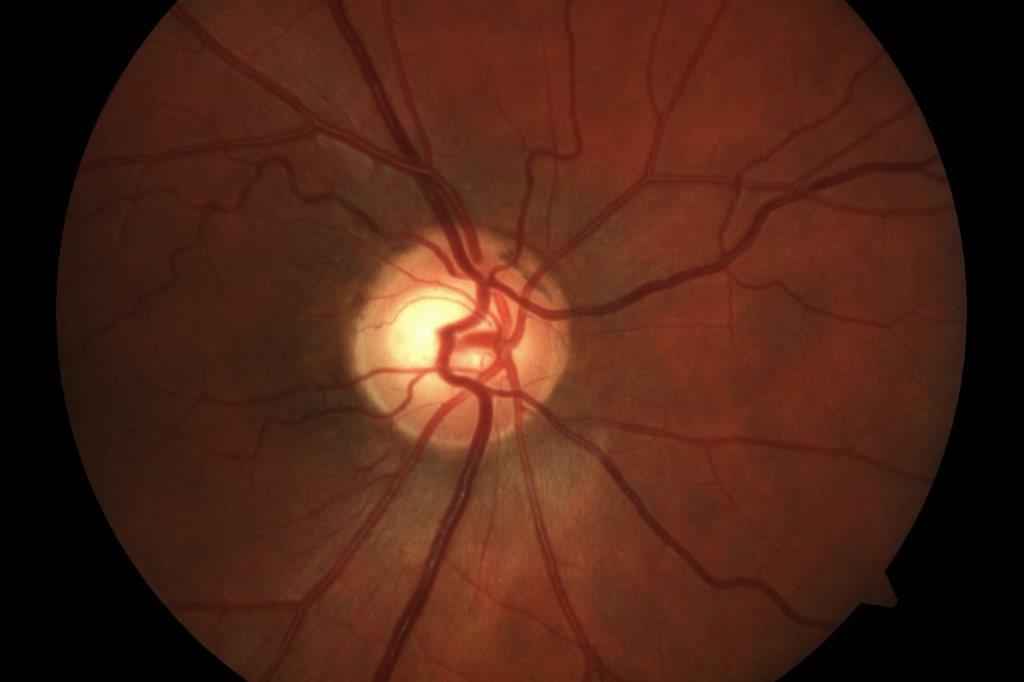
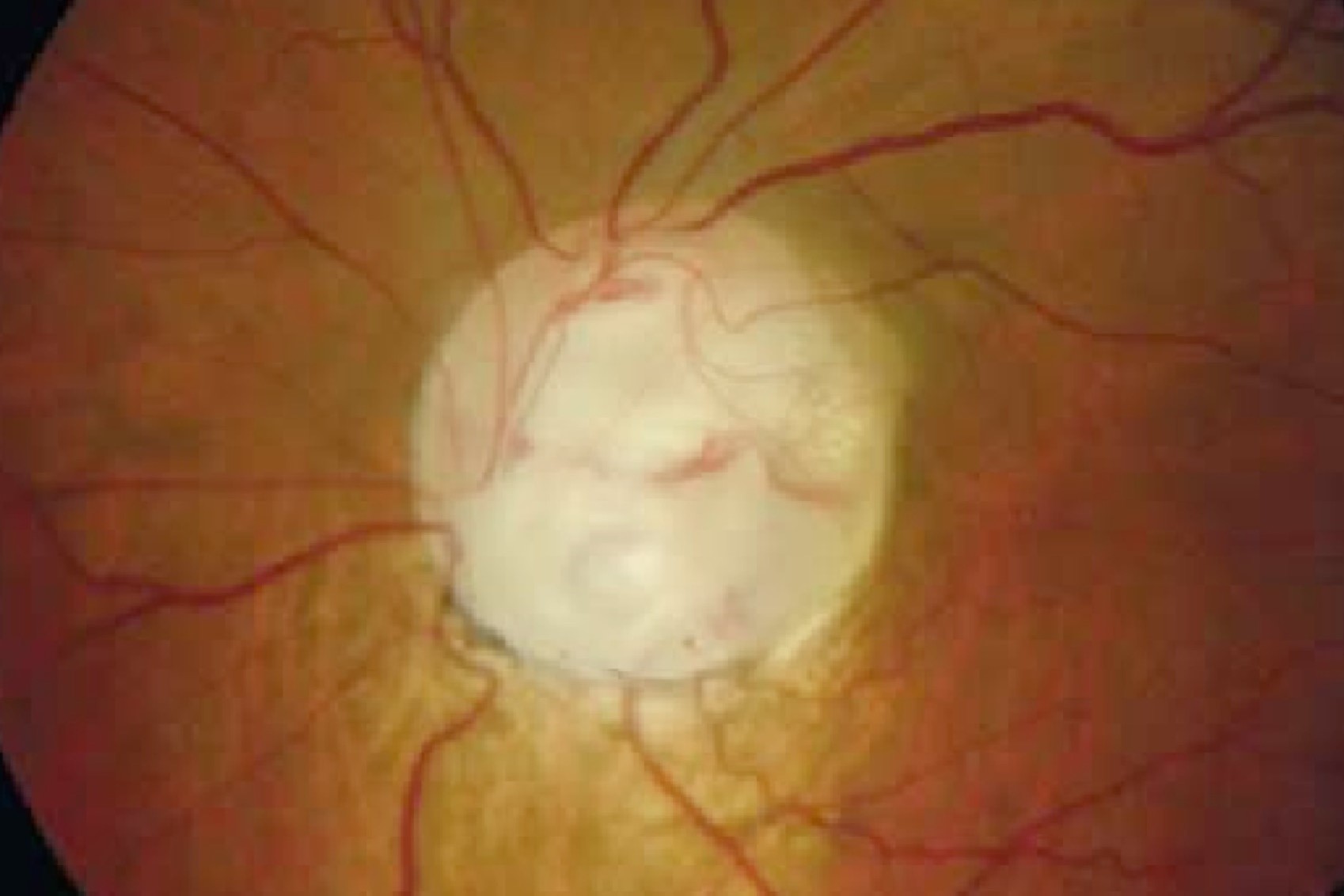
Fig 2 and Fig 3. Congenital optic disc anomalies such as optic disc pit (top) or disc coloboma (below) can sometimes mimic glaucoma
Non-glaucomatous optic neuropathy
Many non-glaucomatous optic neuropathies (Table 1) can be mistaken for glaucoma, at least in their early stages. Compressive optic neuropathies, such as meningiomas and other intracranial tumours, are particularly concerning examples of glaucoma masqueraders and need to be identified early to prevent vision and life-threatening consequences.
In most cases, it’s possible to distinguish between glaucomatous and non-glaucomatous optic neuropathy with careful history and clinical assessment as there are characteristic differences in clinical presentation. These differences are highlighted in Table 2, and the presence of one or more of these red flags when working-up a glaucoma patient (particularly for normal-tension glaucoma) should heighten your suspicion that an alternative diagnosis to glaucoma may be present. Patients with one or more of these red flags need to be referred for further investigation, specifically neuroimaging.
Congenital optic disc anomalies
Congenital optic disc anomalies such as optic disc pit (Fig 2) or disc coloboma (Fig 3) can also sometimes mimic glaucoma due to variable optic disc and VF abnormalities. Often these conditions are diagnosed at an early age and do not change over time, which helps to distinguish them from glaucoma. However, if there is uncertainty, monitoring these patients for progressive change over time is recommended, as this would be more suggestive of glaucoma.
Myopic discs
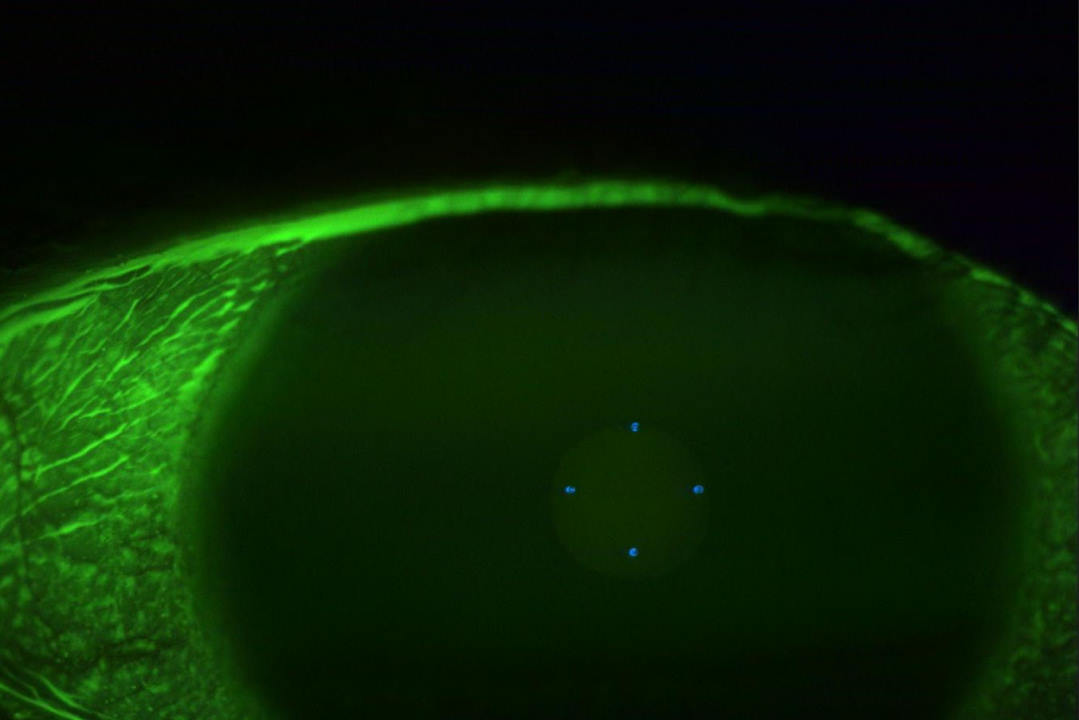
Patients with moderate to high myopia (> 6D) can sometimes have discs that resemble glaucoma (Fig 4). They often demonstrate tilted discs (usually temporally), shallow cupping, pale neuroretinal rims, scleral crescents and peripapillary atrophy similar to glaucomatous discs. Myopic discs do not only masquerade as glaucoma but are also at an increased risk of developing glaucoma. These patients commonly have VF defects, typically related to the direction of tilt and most frequently located superiorly or supero-temporally.
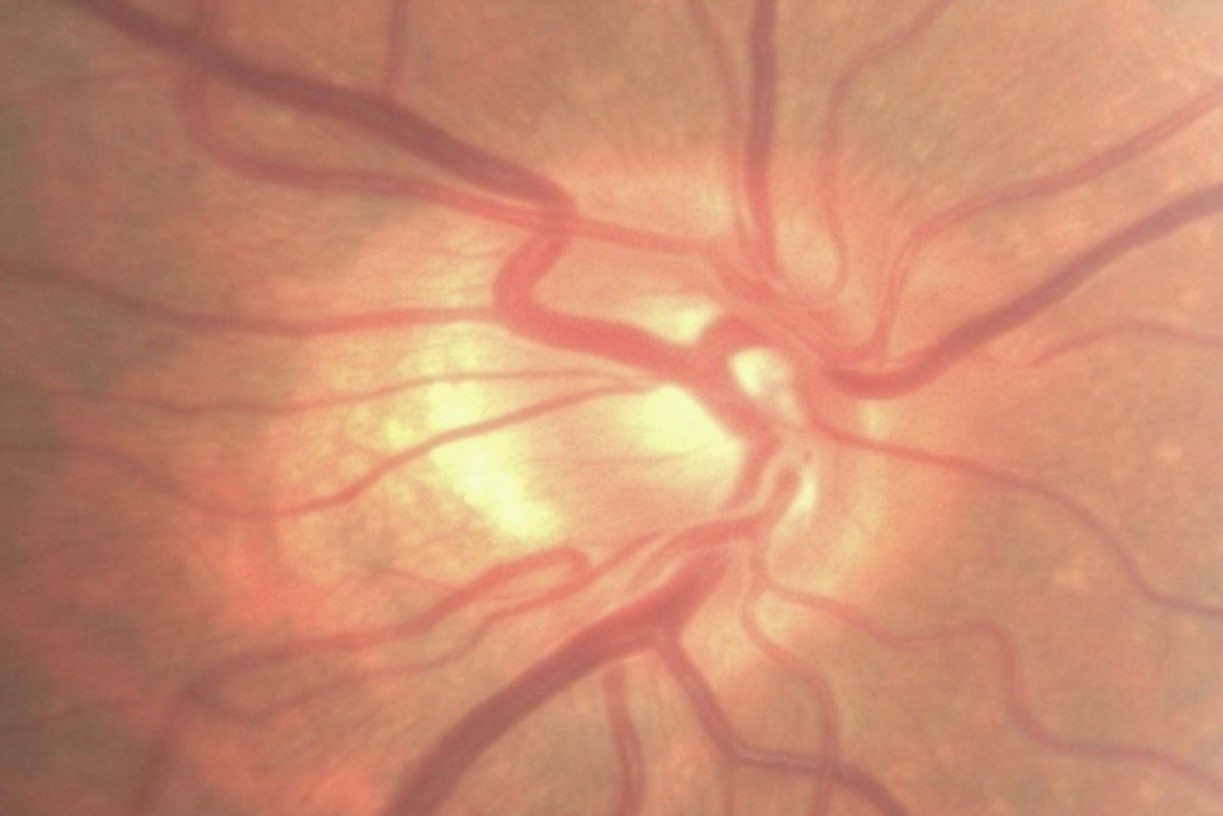
Fig 4. Patients with moderate to high myopia can sometimes have a disc that resemble glaucoma
As with congenital optic disc anomalies, looking for progression over time is important if glaucoma is suspected. In addition, the presence of other risk factors (family history, migraine, Raynaud’s phenomenon, hypotension), level of IOP (borderline vs low, considering central corneal thickness), disc haemorrhage and/or localised notching, and nasal or arcuate VF defects with matching OCT retinal nerve fibre layer-thinning can help identify underlying glaucoma in these patients.
Previous retinal vascular occlusions
A previous branch retinal vein occlusion (BRVO) or branch retinal artery occlusion (BRAO) can sometimes result in localised optic disc cupping with pallor and a VF defect that looks like glaucoma. Following a BRVO, there will usually be associated retinal vascular abnormalities in the distribution of the vein occlusion and possibly collateral vessels to help identify the underlying diagnosis. In cases of previous BRAO, OCT imaging may be helpful and will demonstrate inner retinal thinning that is not usually seen in glaucoma.
Conclusion
It is important to consider potential glaucoma masqueraders when working-up a patient for glaucoma, particularly when the IOPs are normal and the typical glaucomatous findings are not present. Non-glaucomatous optic neuropathies (especially compressive optic neuropathies) are potential glaucoma masqueraders that need to be diagnosed early to avoid vision- and life-threatening complications. Although it can sometimes be challenging to distinguish between glaucomatous and non-glaucomatous optic neuropathy, there are easily recognisable red flags that can help you and being alert to these is vital.
Table 1. Glaucoma masqueraders
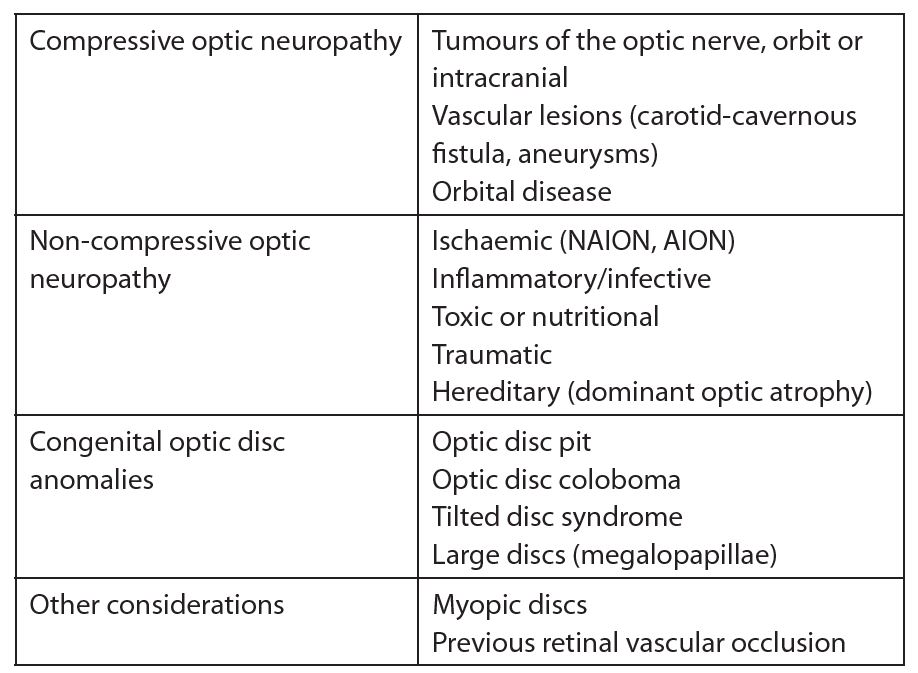
Table 2. Red flags for non-glaucomatous optic neuropathy

Dr Hussain Patel is a consultant ophthalmologist at Greenlane Clinical Centre specialising in glaucoma and cataract surgery. He is also a senior lecturer in ophthalmology at the University of Auckland and works in private practice at Eye Surgery Associates.