Assessing the latest research in myopia control
What a turbulent year 2020 has been for health! We have bravely rallied against invisible viral pathogens, survived the eczema-inducing deluge of alcohol-based hand sanitiser and remained relatively sane despite the monotony of lockdown. However, one disease that we have not conquered here in New Zealand still exists. Worryingly it has probably grown teeth over this winter, wallowing in a perfect growth-medium of home detention and screen-based entertainment: childhood myopia.
Fortunately, this year there is more information and awareness out there in the digital space about myopia and the methods to manage it in our young patients. We are lucky that a significant number of international companies and suppliers have taken up the cudgels and offered virtual webinars on this and other related topics in the last six months. On average, I have tuned into at least one myopia-based education event a month, often led by world leading experts that we would never have had a chance to hear downunder in the pre-Covid world. Yes, I do get a twinge of self-consciousness listening into colleagues while wearing shorts and bare-feet, and yes about an hour or so in to any webinar, despite the quality of the content, the yawns do begin; they are no substitute for a face-to-face conference, but they have great value none-the-less.
In my capacity as vice-president of the Orthokeratology Society of Oceania (OSO), I was recently involved in a particularly good webinar for our members, exploring some of the recent research from three of Australia’s top myopia investigators.
Ortho-k and microbial keratitis
The first presentation was from OSO board member Dr Kathleen Watt, clinic director of the School of Optometry and co-head of the myopia research team at the University of New South Wales (UNSW). Kath offered an update on the work she and her colleagues started in 2007, exploring the safety of orthokeratology (ortho-k) lenses in Australia¹. In this early paper, nine cases of microbial keratitis in ortho-k wearers was reported via questionnaire by OSO members between 1997 and 2005. This questionnaire-based study was repeated recently with the early results discussed.
Although the details cannot be released until they are officially published, some trends can be shared: there was a smaller number of total infections in ortho-k patients reported and none in the past two years. This could reflect a trend amongst ortho-k practitioners to recommend earlier replacement of lenses, typically annually, and anecdotally, the popularity of hydrogen peroxide-based cleaning solutions with ortho-k lenses. Another trend was that most of the infection cases had poor compliance in their history, reminding us to really enforce the three Rs:
- Recall patients appropriately (six-monthly in my clinic)
- Replace lenses (yearly) and cases regularly
- Remind patients of correct techniques (no water, correct solution use, prompt follow-up if symptoms)
Interestingly Kath’s data also showed that when compared to the first study, significantly more of our ortho-k patients these days are younger (<15 years) and of Asian ethnicity, reflecting the adoption of ortho-k as a myopia control strategy in these high-risk groups. We await the fully published data with interest!
How ortho-k slows axial eye growth
The highlight of the night was Queensland Institute of Technology Associate Professor Stephen Vincent’s talk discussing new evidence showing how ortho-k and multifocal soft contact lenses actually slow axial eye growth in myopia. Traditionally, we have thought that these lenses focus peripheral light rays more anteriorly in the retina than traditional spectacles or contact lenses, thus decreasing the stimulus for eye elongation to match the peripheral hyperopic defocus. Stephen explained that despite animal models following this rule, it turns out that relative hyperopic defocus does not predict myopia in humans. Professor David Atchison’s paper from 2015 followed 1700 seven-year-old Chinese children over a two-year period and measured horizontal peripheral refraction under cycloplegia². As relative hyperopic refraction increased, the level of myopia progression was no higher, calling into question the validity of treatments claiming to alter peripheral refraction.
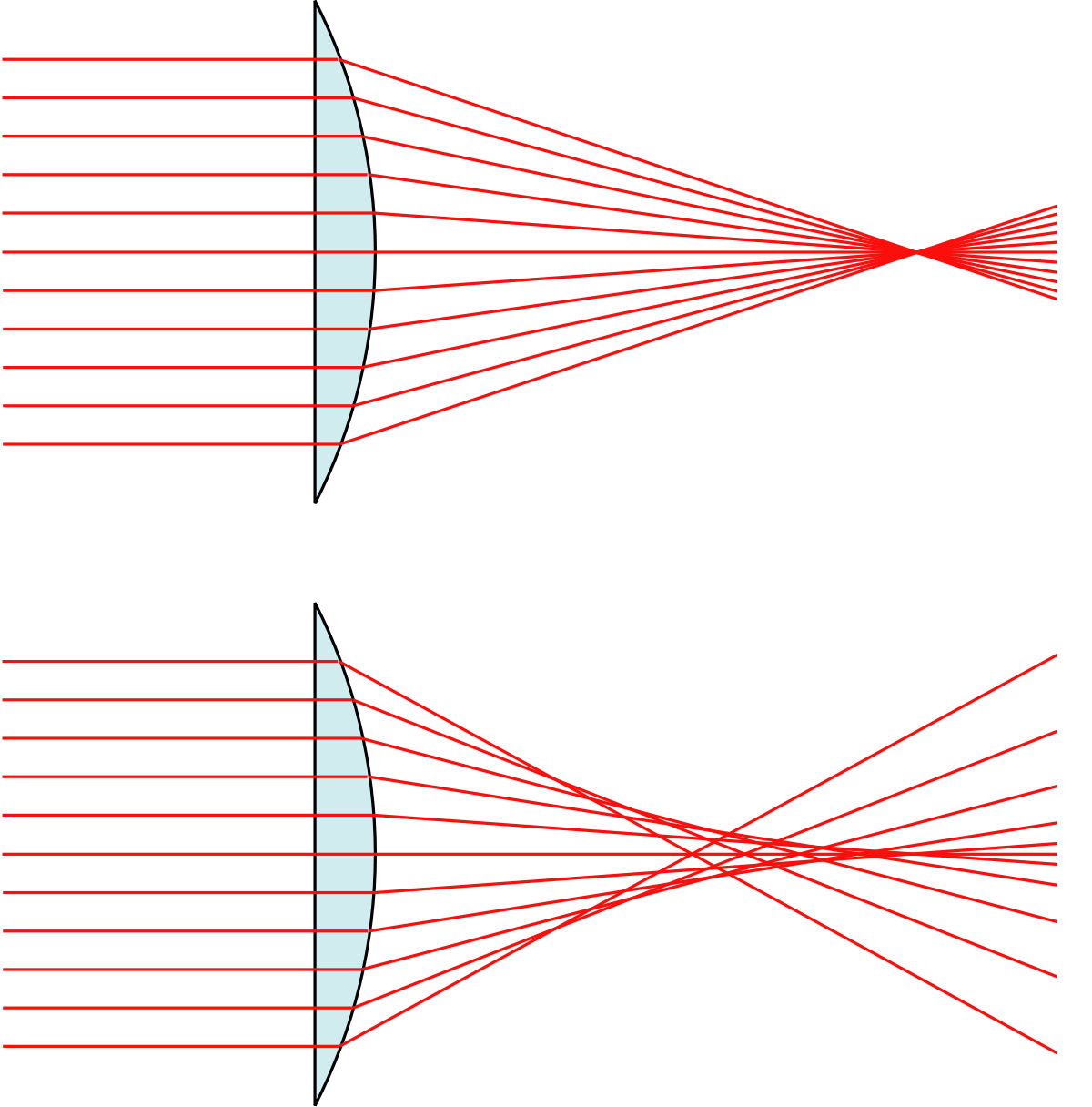
Fig 1. A lens without spherical aberration (top) and with positive spherical aberration (bottom). SA caused peripheral light rays to be focused more anteriorly, occurring more in an eye corrected with ortho-k and myopia-control multifocal contact lenses
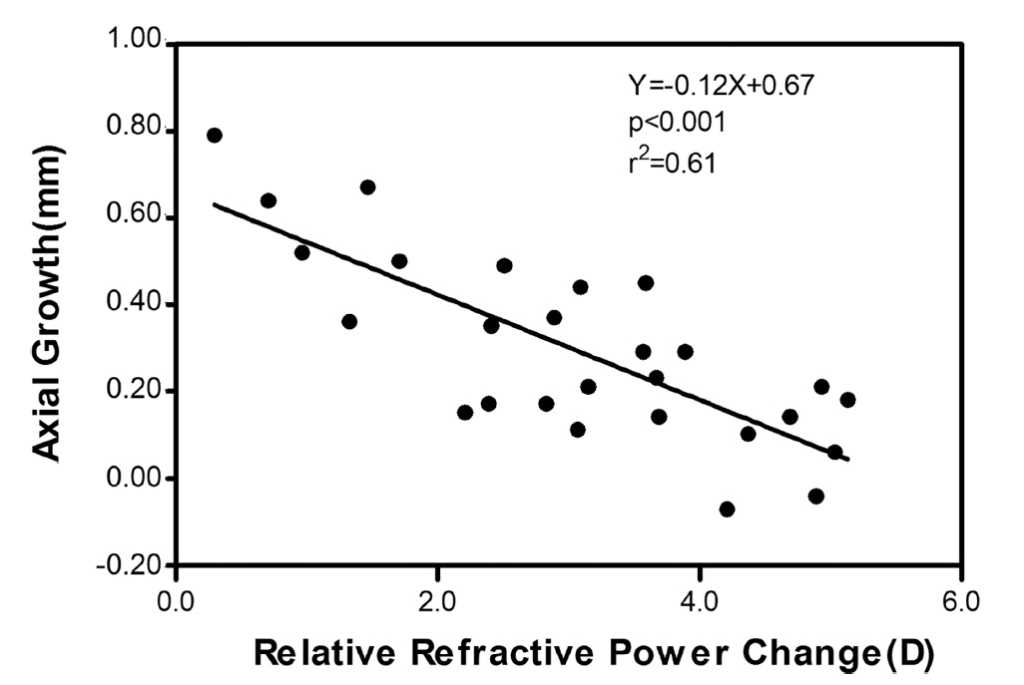
Stephen proposed that higher order aberrations, in particular spherical aberration (SA) (Fig 1), seem to be more important in predicting and affecting axial eye growth. In 2018, his research team showed that children with a higher level of natural positive SA in their eye showed slower eye growth over time³. There is also a number of studies suggesting that inducing a higher level of positive SA with a correction like ortho-k slows eye growth more. Zhong et al showed that the greater the change in corneal power from central to peripheral induced by ortho-k lenses in children (thereby inducing more SA) the slower the eye growth (Fig 2, see main pic above)⁴,⁵. A very recent study by Stephen’s group actually measured the higher order aberration profile of a cohort of ortho-k patients over two years⁶. The higher the level of SA induced by the treatment, the slower the eye growth (Fig 3).
Increasing induced spherical aberration
The next logical question is how can we alter our optical treatments to increase the level of SA induced? It is generally thought that as the baseline level of myopia corrected in ortho-k increases, the higher the level of SA is induced. Stephen’s research team conducted a study to investigate what effect designing an ortho-k lens with a higher compression factor (essentially a flatter base curve to aim for a larger over-correction for the patient) had on SA. They found that increasing the compression factor from a normal level of 0.75D up to a 1.75D overshoot, induced 45% more SA into the system⁷. Anecdotally, in the real world I have found that significant over-correction of myopia with ortho-k can lead to near blur in the morning, asthenopia and decreased quality of vision in some patients, so this strategy does need further refinement.
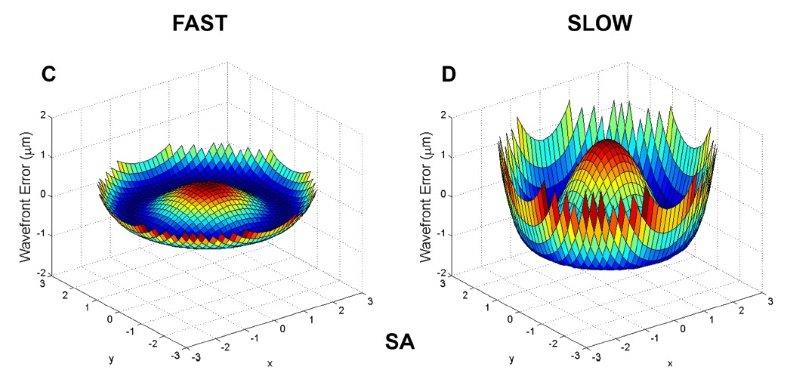
Fig 3. An example of the SA difference profile with ortho-k for a fast axial progressor (left) and a slow axial length progressor (right)⁶
Another way to increase SA in the system is to increase pupil size. The final paper Stephen shared looked at the combination treatment of ortho-k with atropine, an area that is starting to generate some interest. Vincent et al in particular concentrated on the higher order aberrations and found that at six months, the 0.01% atropine and ortho-k group showed a larger photopic pupil size than the ortho-k monotherapy group and slower eye growth (A+OK: -0.01mm +- 0.12mm vs OK: 0.05mm +- 0.08mm)⁸. In terms of a correlation between higher order aberration and axial eye growth the only significant association was found in the combination group. SA appears to be protective against axial length growth, concluded Stephen, a very interesting finding when considering how to create the best myopia control therapy for our patients.
Customising myopia control
Dr Pauline Kang, another UNSW senior lecturer and myopia researcher, ended the webinar on a related theme: exploring ways to customise a myopia control programme for the best results. These days we are blessed with a number of good myopia control options for our patients, with more to come in the form of more novel spectacle lens treatments, such as Hoya’s MiyoSmart lens. But which option is best for each patient and what should you do if the treatment is not working as well as you would like? All studies using myopia control treatments that show a high level of axial growth control, such as the recent DIMS spectacle lens results, the Misight study, a plethora of ortho-k meta-analyses and even the atropine ATOM studies, show a high level of individual variability. Some patients cease progression all together, while myopia in others marches on unperturbed.
Pauline presented results from several studies looking at ways to change your myopia control strategy for improved results. This could involve increasing the mid-peripheral steepening or decreasing the treatment zone size in ortho-k. An early prospective study investigated decreasing the ortho-k optic zone size from 6mm to 5mm, but this did not seem to alter the peripheral refraction level⁹. A more recent study in 2019 confirmed that changing ortho-k lens parameters did indeed create a smaller treatment zone size, but not the peripheral refraction, though measurement artifacts with autorefraction could be responsible for masking an effect¹⁰.
When considering soft contact lens treatments, daily soft contact lenses like Misight and the Naturalvue MF lens cannot be customised yet, however a monthly lens used for myopia control can be - the Biofinity multifocal. Jeff Walline’s group in the BLINK study showed that over three years children using the high add (+2.50) centre-distance multifocal had a slower axial change than a medium add lens (+1.50) and a single vision lens¹¹. Adjusted mean eye growth was 0.42mm for high-add power, 0.58mm for medium-add power, and 0.66mm for single vision. This was consistent with suggestions earlier in the webinar that increasing the ‘add’ and therefore SA may result in better myopia control. Other options for improved myopia control included adding atropine to MFSCL or ortho-k in combination treatment, or increasing the concentration of atropine to 0.025% and 0.05%.
With the increase in awareness and research, it is an exciting time to be managing myopia in children.
For more on this area, visit: https://eyeonoptics.co.nz/articles/archive/2020-year-of-the-orthokeratologist/
References
- Watt KG, Boneham GC, Swarbrick HA. Microbial keratitis in orthokeratology: the Australian experience. Clin Exp Optom. 2007 May;90(3):182-7
- Atchison DA, Li SM, Li H, Li SY, Liu LR, Kang MT, Meng B, Sun YY, Zhan SY, Mitchell P, Wang N. Relative Peripheral Hyperopia Does Not Predict Development and Progression of Myopia in Children. Invest Ophthalmol Vis Sci. 2015 Sep 1;56(10):6162-70
- Lau JK, Vincent SJ, Collins MJ, Cheung SW, Cho P. Ocular higher-order aberrations and axial eye growth in young Hong Kong children. Sci Rep. 2018 Apr 30;8(1):6726
- Zhong Y, Chen Z, Xue F, Zhou J, Niu L, Zhou X. Corneal power change is predictive of myopia progression in orthokeratology. Optom Vis Sci. 2014 Apr;91(4):404-11
- Zhong Y, Chen Z, Xue F, Miao H, Zhou X. Central and Peripheral Corneal Power Change in Myopic Orthokeratology and Its Relationship With 2-Year Axial Length Change. Invest Ophthalmol Vis Sci. 2015 Jul;56(8):4514-9
- Lau JK, Vincent SJ, Cheung SW, Cho P. Higher-Order Aberrations and Axial Elongation in Myopic Children Treated With Orthokeratology. Invest Ophthalmol Vis Sci. 2020 Feb 7;61(2):22
- Lau JK, Vincent SJ, Cheung SW, Cho P. The influence of orthokeratology compression factor on ocular higher-order aberrations. Clin Exp Optom. 2020 Jan;103(1):123-128
- Vincent SJ, Tan Q, Ng ALK, Cheng GPM, Woo VCP, Cho P. Higher order aberrations and axial elongation in combined 0.01% atropine with orthokeratology for myopia control. Ophthalmic Physiol Opt. 2020 Nov;40(6):728-737
- Kang P, Gifford P, Swarbrick H. Can manipulation of orthokeratology lens parameters modify peripheral refraction? Optom Vis Sci. 2013 Nov;90(11):1237-48.
- Gifford P, Tran M, Priestley C, Maseedupally V, Kang P. Reducing treatment zone diameter in orthokeratology and its effect on peripheral ocular refraction. Cont Lens Anterior Eye. 2020 Feb;43(1):54-59.
- Walline JJ, Walker MK, Mutti DO, Jones-Jordan LA, Sinnott LT, Giannoni AG, Bickle KM, Schulle KL, Nixon A, Pierce GE, Berntsen DA; BLINK Study Group. Effect of High Add Power, Medium Add Power, or Single-Vision Contact Lenses on Myopia Progression in Children: The BLINK Randomized Clinical Trial. JAMA. 2020 Aug 11;324(6):571-580

Alex Petty is a New Zealand optometrist based at Bay Eye Care in Tauranga, with a particular interest and knowledge in specialty contact lenses, ortho-k and myopia control. He is vice-president of the Orthokeratology Society of Oceania and a founding member of the NZ Myopia Action Group.